General Advice
Differentiating Between Complications And Negligence
Negligence is a term used by lawyers and not necessarily in the purview of medical practitioners.
From a medical practitioner’s perspective, the term relates to three interlinked activities. The first is the presence or otherwise of a duty of care to the patient. It would be hard to deny that such a duty existed in a clinical liaison.
The second relates to a breach of that duty. From the medical perspective, this can be more difficult to analyse although expert opinions can assist.
The third facet is the establishment of a link between a breach (if it occurred) and an adverse quantifiable outcome.
‘Doctor, you amputated the wrong leg!’
Let’s Look at Some Adverse Outcomes
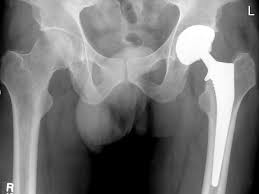
Unfortunately, complications occur and could seemingly fall under the heading or guise of “negligence”. For example, more than 50,000 Australian patients undergo total hip replacement every year. This is an extraordinary number of operative interventions and almost all of them do extremely well. A small but finite percentage does not do well. Almost 1% of patients will have an infection. Of those, 2% or 3% will note ongoing sepsis indefinitely.
A further 1% or so of patients may suffer with an episode of dislocation of the joint. Again, a small subset of that 1% may note recurrent dislocations and require further operative intervention.
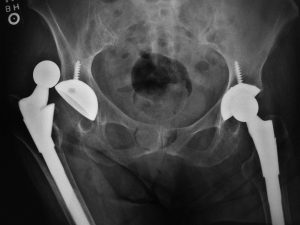
Even more seriously, approximately 2 in 1000 patients undergoing a hip replacement will die. The causes of death are usually of a cardiopulmonary nature and occur presumably and hopefully as a result of factors outside the control of the treating team. Whilst all of these complications are undesirable, they do not necessarily indicate negligence.
Conversely, if a patient suffers with recurrent dislocation of a joint because the implants have been seriously malpositioned, a claim for negligence might exist. Several tests must be applied. The modified Bolam principle will be one. If it can be established that the surgical performance was substantially below that expected of a reasonably competent, appropriately educated hip replacement surgeon in Australia, then the test may be met.
Not all experts are willing to engage in cases of alleged medical negligence. Other experts are prepared to stand up and be counted.
I suggest that you ensure you engage an expert who has the experience, the wisdom and the courage to call it as it really is.
Oh, and be careful of interpersonal differences and TURF WARS!