Lead Article
Future Therapeutic Costs – Who Pays What and When?
Plaintiffs undergoing a medicolegal examination have usually reached a state of Maximal Medical Improvement (MMI) following the index injury or incident. Many months and sometimes years have elapsed and the therapeutic programme, regardless of its complexity, has usually plateaued. Expenditures to date can be accurately quantified. That’s the easy part.
It is more difficult however to accurately assess future therapeutic requirements. An insightful understanding of the natural history of conditions, the ability to formulate an accurate prognosis and experience with all facets of medical costs are required.
There is More to it than Just a Fall
For example, a 58 year old lady may have fallen at the shopping centre and sustained a fracture involving her proximal thigh bone or femur. This is a so-called femoral neck fracture. Varying therapeutic regimens are available for managing this problem but one may have included the performance of a total hip replacement.
Hip replacements perform superbly under normal circumstances. Those performed for femoral neck fractures are less good but still more than satisfactory.
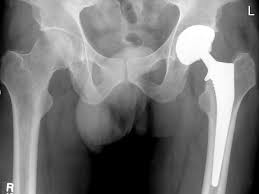
Hip replacements are man-made and not God-made. They have the ability to wear, loosen, fracture and fail. It is a reasonable assumption that hip replacements will not last “forever”.
How Long Will Things Last?
Whilst it is always difficult to predict just how long a specific joint replacement will last in a particular patient, longitudinal studies can give some statistical advice. For example, a well performed hip replacement has a 90% chance of not requiring revision within 20 years. It would be unrealistic to think that all of these joint replacements will fall off the perch in their 21st year. Clearly, that is not the case. Many will last 30 years, some 40 years and there may even be a few still around in 50 years provided the plaintiff lives long enough.
We are all Living Longer
If we come back to our 58 year old plaintiff, and given that she has a further life expectancy of three decades or so, it would be reasonable to assume that she has at least a 15% chance of requiring a revision operation at some time. Revision hip replacements are more complex and more expensive than a primary hip replacement. Costs can be assessed variously but in general terms, a total expenditure in the vicinity of $60,000 can be expected. It may therefore be reasonable to allocate 15% of that $60,000 in her final award.
Costs Can Add Up
Other and less obvious costs can also be involved. She may require the use of a walking stick or a wheelchair. She may benefit from the intermittent ingestion of analgesics with associated pharmaceutical costs. She may require physiotherapy and repeated visits with her local medical officer or her orthopaedic surgeon. All of these factors require appreciation and calculation.
Future therapeutic costs can become a very important part of any settlement following a personal injury or medical negligence claim.